Is the Allurion Program more effective than dieting alone?

In short – Yes! Read on to find out why our holistic 6-month program gives you better results than just dieting alone, and we have the data to back it up!
We know that losing weight is not easy. Not only do you need the right tools and support on your side, very often diet and exercise alone are just not enough to achieve significant weight loss results.
While there are a range of effective and sustainable weight-loss treatments out there, what’s consistent across all of them is taking steps to change your lifestyle habits and behaviors, as well as your diet and physical activity.
In fact, a more holistic lifestyle change approach is recommended around the world as the cornerstone to any weight-loss treatment, even medical or surgical options (Ref:1-7). It’s the combination of all these elements that delivers optimal results, not doing any of them in isolation.
Did you know that the Allurion Program leads to nearly 2.5 times the weight loss than a lifestyle change program alone?
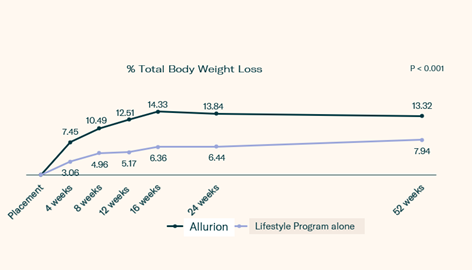
Research shows that the Allurion Program (a combination of our unique swallowable gastric balloon and a supported lifestyle change program) achieves significantly better results than a lifestyle change program alone. (Ref:8) Other studies on intragastric balloons tell the same story; they help patients achieve significantly superior weight loss vs just dieting alone. (Ref:9)

Unsuccessful weight loss methods
As Zoe Griffiths (Registered Dietitian and Director of Global Nutrition at Allurion) highlights, what’s worrying is that not only have the majority of adults tried to lose weight in the last 12 months (depending on the county it could be anything from 50-80%)10,11 , but that most are unsuccessful. Studies underscore the need for increased support and solutions for weight management.
One study11 shows that the most common weight loss methods people use are calorie-controlled or restricted diets (72% of participants), exercise programs or courses (22%), and pharmaceutical treatments (12%). However, three-quarters of participants who attempted to lose weight within the past year, did not achieve a clinically meaningful weight loss defined as at least 5% of their body weight.
In another study10, the most commonly reported weight loss methods were exercising (63%) and eating less food (63%), followed by consuming more fruits, vegetables, and salads (50%).
The evidence clearly shows that exercise and calorie-controlled or restricted diets are the least beneficial, with respect to achieving clinically meaningful weight loss. These isolated methods alone are not enough.
How the Allurion Balloon and Allurion Program lead to successful weight loss
The swallowable Allurion Balloon is the only gastric balloon in the world that requires no surgery, no endoscopy and no anesthesia*. This non-invasive medical tool kick-starts your weight loss by:
. Helping you feel fuller for longer
. Helping you feel fuller quicker with smaller portions
. Slowing down digestion so you feel less hungry
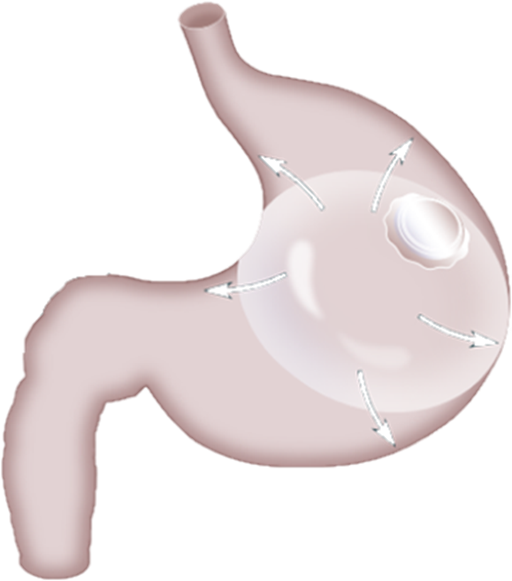
With these benefits on your hunger and satiety, adopting changes to your diet and activity is much easier while you work with your Allurion care team to start making sustainable changes to your lifestyle and eating habits.
As part of the Allurion Program, you will also be provided with an Allurion Connected Scale, Allurion Health Tracker and Allurion App. You can use these to check in with your healthcare team, receive support and guidance, and be accountable for your weight-loss achievements.

This multi-disciplinary approach has led to significant weight loss success for our patients all around the world. On average, our patients lost 10-15% of their total body weight within 16 weeks of having the balloon,12-13 and up to 95% of weight loss may be sustained one year after
the balloon has passed. (Ref:14)
Discover some of our success stories here, and book a free consultation with one of our advisors today!
References
1. Behavioral Weight Loss Interventions to Prevent Obesity-Related Morbidity and Mortality in Adults: US Preventive Services Task Force Recommendation Statement.US Preventive Services Task Force., Curry SJ, Krist AH, Owens DK, Barry MJ, Caughey AB, Davidson KW, Doubeni CA, Epling JW Jr, Grossman DC, Kemper AR, Kubik M, Landefeld CS, Mangione CM, Phipps MG, Silverstein M, Simon MA, Tseng CW, Wong JB. JAMA. 2018 Sep 18; 320(11):1163-1171.
2. Wadden TA, Tronieri JS, Butryn ML. Lifestyle modification approaches for the treatment of obesity in adults. Am Psychol. 2020;75(2):235-251. doi:10.1037/amp0000517
3. Garvey WT, Mechanick JI, Brett EM, Garber AJ, Hurley DL, Jastreboff AM, … Reviewers of the AACE/ACE Obesity Clinical Practice Guidelines. (2016). American Association of Clinical Endocrinologists and American College of Endocrinology comprehensive clinical practice guidelines for medical care of patients with obesity. EndocrinePractice, 22(Supplement 3), 1–203.
4. Jensen MD, Ryan DH, Donato KA, Apovian CM, Ard JD, Comuzzie AG, … Yanovski SZ (2014). Guidelines (2013) for managing overweight and obesity inadults. Obesity, 22(S2), S1–S410.
5. World Health Organization. (1998). Obesity: Preventing and managing the global epidemic (Publication No. WHO/NUT/NCD/98.1). Geneva: Author.
6. NICE Obesity: identification, assessment and management. Clinical guideline [CG189]Published: 27 November 2014
7. Weight management: lifestyle services for overweight or obese adults. Public health guideline [PH53]Published: 28 May 2014
8. *Results at 16 weeks. Raftopoulos, I et al Holyoke Medical Center. Holyoke, MA An Intensive 52 Week Nutritional, Exercise and Behavior Modification Program: Comparing With or Without the Allurion IGB Presented at ASMBS 2019
9. Genco A, Balducci S, Bacci V, et al. Intragastric balloon or diet alone? A retrospective evaluation. Obes Surg. 2008;18(8):989-992. doi:10.1007/s11695-007-9383-9
10. Products - Data Briefs - Number 313 - July 2018 (cdc.gov)
12. Ienca et al. Obes Surg. 2020 Apr;30, pgs 3354–3362
13. Vantanasiri et al. Obes Surg. 2020, 30, pgs 3341–3346



